External hemorrhoid skin tag1/1/2024 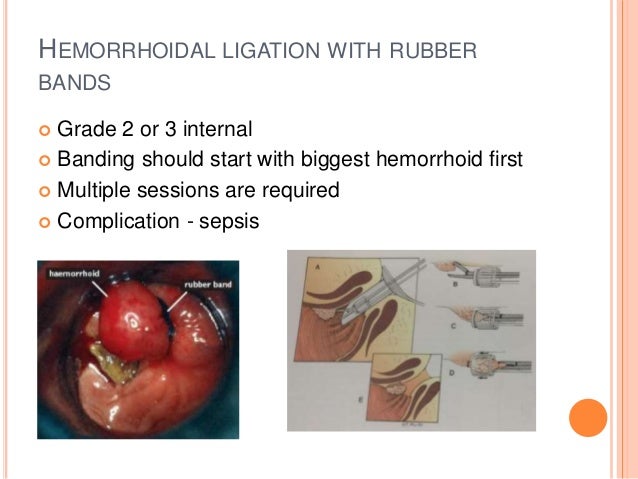
What’s the difference between a skin tag and a hemorrhoid? Before removal, the anal area will be cleaned thoroughly. 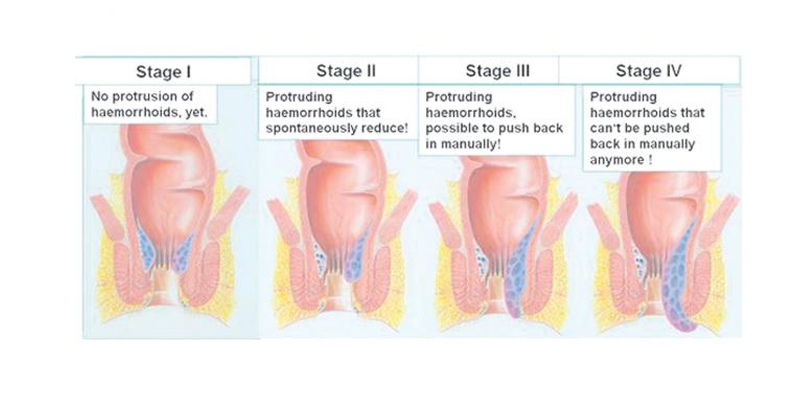
They may also provide a sedative, depending on the treatment. The procedure is generally painless as the doctor will inject a numbing medication around the external anal skin tag to reduce pain. 
12.People also ask What should I expect during the removal of anal skin tags? Pain, urinary retention and recurrence are common postoperatively. Even those who undergo surgery cannot be guaranteed of a good result. The outcomes for most people who do not change lifestyle are not satisfactory. Only via an interprofessional approach can the morbidity of hemorrhoids be reduced. These simple measures not only reduce the risk of hemorrhoids but also decrease healthcare expense. The primary care clinicians and nurses should educate the patients on the need to change lifestyle to prevent hemorrhoids this means becoming physically active, eating a high fiber diet, drinking ample water, taking a stool softener, reducing body weight and avoiding prolonged seating. Many patients do have residual anorectal pain after surgery. While surgery is effective, the results are not optimal and recurrences are common. Other minimally invasive options include sclerotherapy and infrared photocoagulation. Rubber band ligation is a minimally invasive treatment option for first, second, and some third-degree internal hemorrhoids that do not respond to conservative therapy. This includes increased dietary fiber, stool softeners, and increased water intake. The primary care provider, pharmacist, and nurse practitioner play a vital role in educating the patient on preventing these lesions.Ĭonservative therapy is considered first-line treatment for symptomatic hemorrhoids. Hemorrhoids are best managed by an interprofessional team that includes an emergency department physician, general surgeon, gastroenterologist, and an internist. Today, the aim of treatment is to prevent hemorrhoids in the first place. Over the years, many treatments have been developed to manage hemorrhoids but none is perfect. Patients with a family history of cancer, or patients older than 49 years of age, should be scheduled for a routine colonoscopy.Įxternal hemorrhoids affect millions of people and even though not life-threatening can seriously affect the quality of life. If bleeding is obviously originating from hemorrhoid disease in a young, otherwise healthy patient, the complete colonic examination may be deferred in favor of a close follow-up. Malignancy is a potential cause of blood per rectum that must be considered. Offending microbes include Chlamydia trachomatis, Neisseria gonorrhoeae, and Herpes simplex. Anal intercourse can result in proctitis that yields pain, bleeding, and even skin changes. Although rather uncommon, anal prolapse typically presents with pain during defecation, and the patient may report a palpable mass. These have the potential to result in life-threatening sepsis. Anorectal abscesses can yield severe rectal pain, and sometimes a palpable mass. For example, anal fissures occur in the lower portion of the anal canal and typically yield pain and bleeding, worse with defecation. When considering hemorrhoid disease as a diagnosis, one must give specific consideration to other potential anorectal pathologies. A pressure dressing should be applied and the patient should be asked to undertake sitz baths. The acutely thrombosed external hemorrhoid can be excised under local anesthesia. Post-operative pain is typically managed with oral narcotics, NSAIDs, and sitz baths. In otherwise healthy patients, hemorrhoidectomies can be performed as "same day" surgeries. The persistent or severe disease can be managed operatively, with surgical hemorrhoidectomy. 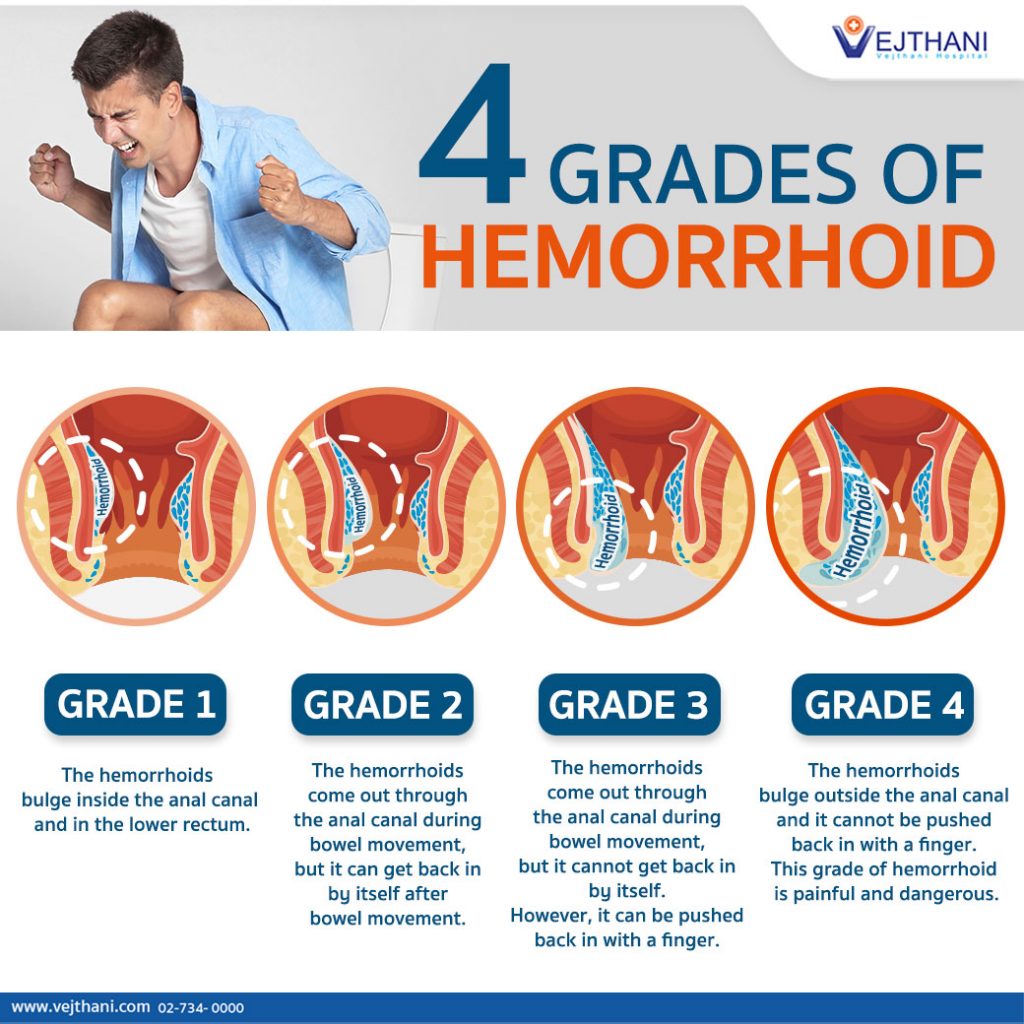
Rubber band ligation is a minimally invasive treatment option for first, second, and some third-degree internal hemorrhoids that do not respond to conservative therapy. Other minimally invasive options include sclerotherapy and infrared photocoagulation. This alleviates congestion and allows hemorrhoid cushions to return to their natural, non-pathologic state. These conservative medical measures can decrease straining and the sheering pressure associated with passing stool. Docusate is an anionic surfactant that promotes water and lipid entry into the stool, thereby softening it. Polyethylene glycol is an osmotic laxative that softens stool by increasing the water content of stool. Of note, the fiber must be accompanied by adequate water intake to ensure that stool is not just bulky, but also soft. Conservative therapy is considered first-line treatment for symptomatic hemorrhoids.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
